Horses have a normal “locking mechanism” associated with their stifle area that allows them to maintain limb extension without considerable muscular effort. This mechanism is called a “stay apparatus” and primarily involves the patella (knee cap), the bottom end of the femur (medial trochlear ridge), and three distal patellar ligaments (ligaments that attach to the knee cap and tibia below the stifle). Horses also have a stay apparatus in the front limb and therefore have the ability to sleep while standing. The horse’s stay apparatus is perfectly normal.
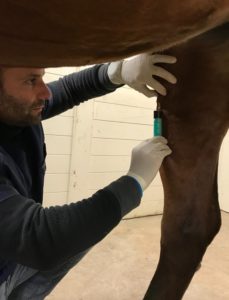
Intermittent Upward Patellar Fixation
The problem arises when this locking mechanism inadvertently occurs (or “catches”) during movement. It generally results in a hypometric (toe-dragging) gait with a delayed forward phase to the stride
That horses with intermittent upward fixation the patella may develop chronic, low-grade lameness due to stifle soreness and may be reluctant to work on soft, deep surfaces or up or down hills. Decrease in the strength of the hind limbs with the consequent loss of performance.
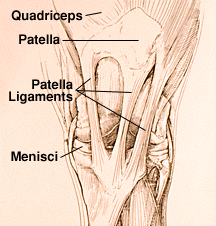
Intermittent Upward Patellar Fixation
Treatment
Corrective shoeing; The idea to is minimize any conformational disadvantages that make IUPF more likely to occur.
Fitness training/ hill work; In our opinion, your horse’s performance will improve dramatically with fitness training. Since we are specifically interested in strengthening the muscles and ligaments associated with the distal patellar (stifle) apparatus.
If your horse improves with fitness training, but behavioral resistance persists as a result of his/her frustration. In some cases, we elect to treat horses exhibiting clinical signs of intermittent upward patellar fixation (IUPF) with estrogen. As you know, estrogen is a naturally-occurring hormone that is present in all horses (both male and female).
However, we do often utilize estrogen as a treatment strategy for IUPF, particularly when there is a considerable behavioral component to the problem.
IUPF is generally very frustrating to the horses, represented by frequent bucking, bolting, spinning, kicking, etc. Since estrogen is also a very competent behavior-modificator, we recommend it for horses that exhibit behavioral problems (anxiety, nervousness) or resistance (such as with IUPF). It seems to help the horses to “relax” and work through the problem more efficiently and safely.
Your horse gets very fit but the problem persists. In these cases, we generally elect injection on the ligament or surgical intervention or combine both techniques. Both techniques are performed in the standing (sedated) horse at the barn;
The first technique is called fenestration or “splitting”. As you may know, the technique involves splitting or separating the ligament fibers within the medial (inside) and middle distal patellar ligaments. This creates defects within the ligament which fills in with scar tissue. As the scar tissue matures and organizes, it contracts, thereby shortening the ligament and repositioning the patella (or kneecap).
The second technique involves infusing a counterirritant (or “blister”) to irritate the tissues and accentuate ligament contraction. As originally described, the technique consisted of infusing the counterirritant (usually 2% iodine in almond oil) adjacent to the medial and middle distal patellar ligaments. With irritation/ inflammation of these tissues we inevitably cause the formation of scar tissue. With maturity, the scar tissue contracts thereby shortening the ligaments and surrounding tissues. The patella is repositioned in a location whereby IUPF is less likely to occur.
We have had the most success performing a technique that combines the splitting and blistering strategies. Rather than split the fibers with a scalpel blade, we simply split them using an 18-gauge 1.5″ needle. Consequently, no external (skin) incision is required. As we remove the needle from between the ligament fibers we infuse a small amount (or trail) of counterirritant into the remaining defect or tract. This stimulates the developing scar tissue to contract even further than it would on its own.








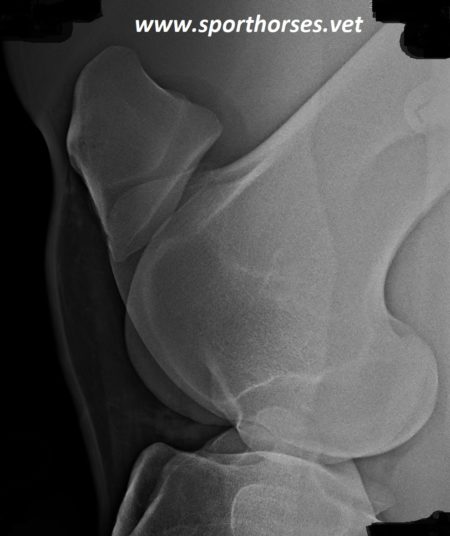
No Comments